Conjunctivitis in children
Conjunctivitis ("red eye" or "pink eye") is a common eye condition that affects children, especially under 5 years of age. It can either be caused by an infection or by an allergy. Infectious conjunctivitis is contagious and may spread to other household members. Allergic conjunctivitis is more common in children with allergies such as hay fever.
Symptoms of conjunctivitis include:
- a red or pink eye (or both eyes)
- redness behind the eyelid
- swelling of the eyelids, making them appear puffy
- excessive tears
- either a watery discharge or a yellow-green discharge from the eye which dries when your child sleeps, causing crusting around the eyelids
- a dislike of bright lights (photophobia)
- a gritty feeling (like there is sand in the eye)
- itchiness of the eyes and eye rubbing
- children with allergic conjunctivitis almost always rub their eyes excessively. They may also have an itchy or runny nose and sneezing
When should you worry?
If your child has any of the following:
- Becomes pale, mottled and feels abnormally cold to touch
- Is going blue around the lips
- Too breathless to talk / eat or drink
- Has a fit/seizure
- Becomes extremely agitated (crying inconsolably despite distraction), confused or very lethargic (difficult to wake)
- Develops a rash that does not disappear with pressure (see the 'Glass Test')
- Is under 3 month of age with a temperature of 38°C / 100.4°F or above
You need urgent help.
Go to the nearest Hospital Emergency (A&E) Department or phone 999.
If your child has any of the following:
- Severe pain in eyes
- Extreme sensitivity to light (photophobia)
- Changes in vision including flashing lights (vision can appear blurred or misted because of discharge smeared over the surface of the eye, but this will usually clear on blinking or wiping the eyes)
- If you notice any redness, swelling or puffiness around the eye or eyelids.
- Severe headache
- Persistent vomiting
- Blisters develop on the skin next to the eye
- Babies under 28 days with a red eye(s) or lots of pus from their eye(s) - note although a sticky eye due to a blocked tear duct is a very common condition in babies (and does not require medical review), this condition does not cause a red eye
- Is finding it hard to breathe
- Seems dehydrated (sunken eyes, drowsy or not passed urine for 12 hours)
- Is becoming drowsy (excessively sleepy) or irritable (unable to settle them with toys, TV, food or picking up) - especially if they remain drowsy or irritable despite their fever coming down
- Has extreme shivering or complains of muscle pain
- 3-6 months of age with a temperature of 39°C / 102.2°F or above (but fever is common in babies up to 2 days after they receive vaccinations)
- Continues to have a fever of 38.0°C or above for more than 5 days
- Is getting worse or if you are worried bacterial conjunctivitis does not improve after 24 hours of antibiotic use
You need to contact a doctor or nurse today.
Please ring your GP surgery or call NHS 111 - dial 111.
If none of the above features are present
Additional advice is also available to young families for coping with crying of well babies – click here.
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111 – dial 111.
Sticky eye in a baby/blocked tear duct - no treatment required (green)
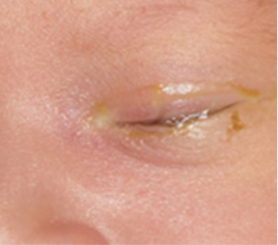
Mild conjunctivitis - no treatment required (green)
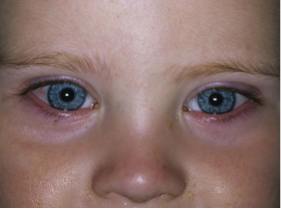
Peri-orbital cellulitis - needs same day review (amber)
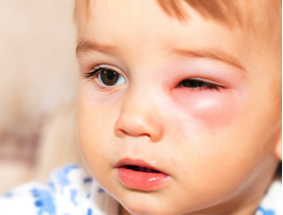
Causes of conjunctivitis
Most cases of conjunctivitis in children are caused by an infection; your child may also have a runny nose, cough or earache.
Treatment
Most children with conjunctivitis do not need treatment with antibiotics - it takes the same amount of time to get better whether an antibiotic is used or not.
If your child has any features of severe infection (amber or red features above), they will need to be urgently seen by a healthcare professional who may decide that your child may benefit from antibiotic treatment. If your child is under 28 days of age and has a red eye(s) or large amounts of pus discharging from their eye(s), they need to be seen by a healthcare professional.
You can help relieve symptoms by gently cleaning the eye(s) with cotton balls soaked in warm water.
- Clean in one direction only, outwards from the inside (nose side) of the eye. This prevents the other eye becoming infected if only one eye is affected.
- Discard the cotton ball each time to prevent reinfection.
- Do not try to clean inside the eyelids as this may cause damage to the inside of the eye. Lubricating eye drops such as 'artificial tears' may give some relief.
- If your child wears contact lenses, make sure they stop using them until their symptoms have completely gone.
It can take up to 2 weeks for a child to fully recover from conjunctivitis . If your child is not improving after 2 weeks, you should take your child to see their GP.
Prevention
- To avoid conjunctivitis spreading to other family members, make sure all family members (and your children) wash hands regularly with warm soapy water and wash your child's pillows and face cloths in hot water and detergent. Avoid sharing towels and pillows.
Your child does not need to be excluded from school or childcare if they have conjunctivitis.

