Poisoning/ accidental swallowing
Poisoning is the harmful effect that occurs when a toxic substance is swallowed, inhaled (breathed in), or comes into contact with the skin, eyes, or mucous membranes such as those of the mouth or nose.
If your child has swallowed an object (i.e. battery, coin, magnet – please click here to be redirected to the correct page. Accidental swallowing of potentially toxic substances occurs most commonly in young children (toddlers), accounting for about 2 in every 100 emergency presentations to hospital.
Products commonly resulting in exposure or ingestion include medicines and household/garden products such as soaps, detergents, garden chemicals.
When should I worry?
If your child has any of these symtoms:
- Unconscious/lethargic
- Confused/agitated
- Has a fit/seizure
- Becomes pale, mottled or blue
- Choking/breathing difficulties
- Severe abdominal pain
- Difficulty swallowing
- Eye pain or redness
You need urgent help.
Go to the nearest Hospital Emergency (A&E) Department or phone 999
If your child has any of these symtoms:
- Rash or skin irritation
- Vomiting/mild abdominal pain
- Headache
If the substance is:
- A medication
- The bottle/packet suggests seeking medical help or has any warning symbols
You need to contact a doctor or nurse today.
Please ring your GP surgery or call NHS 111 - dial 111
Your child has no symptons and has ingested a non harmful substance.
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111 – dial 111
Information to help the health professional - Substance:
1) What substance has your child swallowed or come in contact with?
2) When was the substance taken? How long ago?
3) What was the type of exposure? Did they swallow, inhale, lick it etc?
4) How much of the substance was taken?
Information to help the health professional – your child:
1) Age and estimated weight of your child
2) Any existing medical conditions
3) Any medications or ongoing treatments
4) Any allergies
What should you do after seeking advice or being discharged from hospital:
1) Please monitor your child over the next 24-48 hours.
2) Let them eat or drink normally.
3) Please follow the steps above if any concerns about your child.
4) Please read the following ‘prevention is better than cure’ advice
Prevention is better than cure
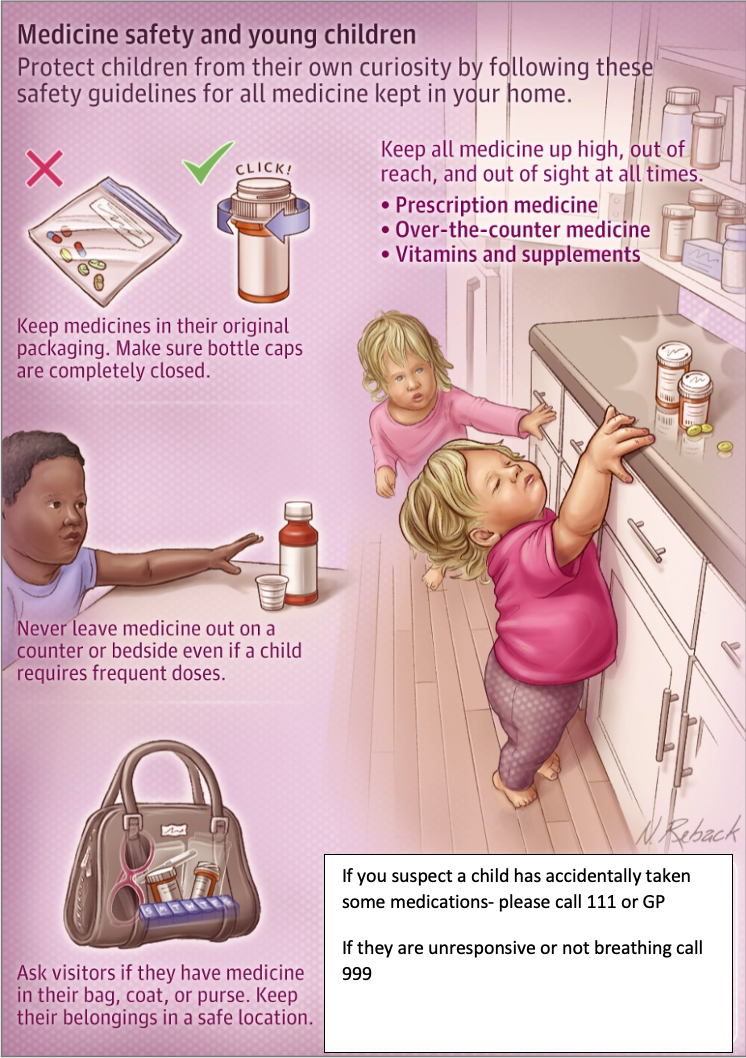
The best way to prevent accidental swallowing or exposure is to limit access to these substances. Whilst children are clever and seem to get hold of anything and everything, by following the advice below you will have done all you can to reduce this risk, just remember the ‘keep SAFE 6 rule’:
Safe Storage – out of reach and out of sight. This includes medications, infuser oils, vape liquids, perfumes and washing liquid/tabs
Safe Containers – keep medications locked away and ensure safety caps are on
Safe Labels – keep medicines in original packaging
Safe Use – use medications and products as directed, and never pretend they are sweets
Safe Disposal – pharmacy for medicines and other products as directed on packaging
Safe Home - install a carbon monoxide detector in your home, ensuring it’s working properly and replace the batteries when needed
Further information can be found in: accidents and injuries - keeping your home safe
For wear and tear, minor trips and everything in between.
Self-care
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
Pharmacists are experts in many aspects of healthcare and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment and many have private consultation areas, so they are a good first port of call. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand - watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand – watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.


